If you are exhibiting symptoms indicating pleural effusion, such as a chronic cough, shortness of breath, or chest pain, Top NYC Pulmanologist Marc Bowen may recommend that you undergo a pleurocentesis procedure (also known as a thoracentesis) in order to accurately diagnose your condition, relieve your symptoms, and improve lung function. An in-office chest ultrasound may be necessary first to determine if there is fluid in the pleural space.
Our NYC pulmonology practice is equipped with the newest state-of-the-art equipment to provide the highest quality patient care. Schedule an appointment with Dr. Bowen or call 212-480-4062 for evaluation and treatment of your breathing issues. Appointments will be confirmed by office staff.
What is Pleurocentesis?
A pleurocentesis, also known as a thoracentesis or pleural effusion treatment, is a procedure used to remove excess fluid from the pleural space (the space between the lungs and the wall of the chest) for diagnostic or therapeutic purposes. Typically, the pleural space is filled with a small amount of fluid, but fluid may accumulate in your chest cavity for various reasons, creating a condition called pleural effusion.
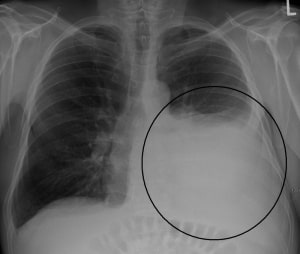
How is a Thoracentesis Performed?
In conjunction with a pleurocentesis, a pulmonologist may take a sample of the pleural fluid or a small piece of tissue from the outer pleura for testing. Testing will help to confirm or rule out infections or diseases such as cancer, pneumonia, congestive heart failure, or pulmonary hypertension.
Dr. Bowen performs the thoracentesis procedure in a hospital setting. Pleural effusion involves injecting a local anesthetic between your ribs in the area where fluid was specifically located via an ultrasound. Next, a needle will be inserted through the ribs and into the chest wall using ultrasound guidance. Using the needle, one of NYCs best pulmonologist, Dr. Marc Bowen, will slowly withdraw the pleural fluid and, if necessary, will send a sample to the laboratory for analysis. In cases where a more detailed pleural biopsy is necessary, Dr. Bowen will use a biopsy needle with a small hook at the end that can take a tiny tissue sample from the outer pleura.
What are the Advantages of a Pleurocentesis?
- Can be helpful in relieving symptoms such as shortness of breath, coughing, and hypoxemia (low oxygen levels)
- Provides valuable information that can be used to diagnose infectious problems, inflammatory problems, and cancer
- Performed using ultrasound guidance to determine the optimal location for inserting the needle to remove fluid and gather a sample
- Only requires the use of local anesthetic
How Much Fluid is Removed During a Thoracentesis Procedure?
The amount of fluid your doctor removes during this test may be dependent upon the goal of the procedure. If the purpose is to discern why you're experiencing pleural effusion, your thoracentesis may remove only a couple of ounces of fluid. If, on the other hand, the goal is to help relieve the symptoms caused by the pleural effusion, such as shortness of breath, then they may remove 20 to 40 ounces of fluid. This is a detail that Dr. Bowen can discuss with you well before your test so you know what to expect.
How Does the Doctor Know Where to Insert the Catheter for Thoracentesis?
You may have undergone a chest x-ray to help Dr. Bowen diagnose your pleural effusion. Another chest x-ray may be done between your consultation and your thoracentesis. This can serve as a guide for the insertion of the needle or catheter that will remove the excess fluid. Alternatively, the doctor may use ultrasound guidance when possible. This painless form of imaging displays with great accuracy where fluid is trapped in the lung space. Fluid may be trapped in several small pockets, all of which can be visualized in the ultrasound.
Can Home Remedies Help Get Rid of Fluid in the Lungs?
If you're dealing with the symptoms of pleural effusion, such as shortness of breath and a dry, nonproductive cough, you may be tempted to look for remedies. It's not difficult to find them. However, we don't recommend using them as an alternative to seeing your doctor. Fluid in the lungs isn't a small issue; it can be a sign of another condition that needs treatment. This is why thoracentesis may be necessary. Home remedies may temporarily reduce your symptoms but they may not resolve the underlying problem. In fact, if you rely on home remedies for the symptoms of pleural effusion, you miss the opportunity to receive early, potentially life-saving care.
Why Is Thoracentesis Needed to Diagnose Pleural Effusion?
It isn't enough to know that you've got "water on the lungs." Your doctor has to discern why this is happening so you can receive the appropriate level of care. Thoracentesis is how we do this. Taking a sample of the fluid and sending it to the lab, Dr. Bowen can determine if the fluid is protein-rich (exudative) or protein-poor (transudative). This is helpful because each measure can lead your healthcare team to the cause of your pleural effusion. For example, protein-rich fluid can point to kidney disease, pneumonia, inflammatory disease, or cancer. Protein-poor fluid could point to cirrhosis, heart failure, or may be a lingering effect of open heart surgery.
What is the Recovery from Thoracentesis Treatment?
After undergoing a pleurocentesis procedure, Dr. Bowen will send out any samples taken during the procedure for testing. Directly following the procedure, additional chest imaging may be necessary to ensure no complications. With the pleurocentesis results, Dr. Bowen will be able to make a diagnosis and explain the next steps for treatment. In most cases, recovery is quick and patients are able to go home the same day.
Read What Our Patients Are Saying!
"Dr. Bowen is very thorough and attentive. He truly cares about your well being. He is very detail oriented and makes certain that you understand your diagnosis and treatment plan."
Schedule Your Pleurocentesis Treatment Today!
For an appointment or for more information about pleurocentesis and pleural effusion treatment, call 212-480-4062 to schedule an evaluation with Dr. Marc Bowen.